Contents
In this month's newsletter:
- NHS South Yorkshire Winter Covid & Flu Vaccinations Campaign Communications Toolkit 2025
- Supporting people with a Learning Disability, Autistic people, and people with Severe Mental Illness (SMI) to get their winter vaccines
- NHS England launches Medium Term Planning Framework
- NHS South Yorkshire Interim CEO appointment
- Review of GP funding formula announced
- Improving Outcomes for People with a Learning Disability
- Expansion of the NHS Pharmacy Contraception Service – updated service specification and patient group directions
- Webinar for employers of Physician/Anaesthesia Associates
- Bassetlaw Hospice: Transfer of services
- Digital pathways for follow-up with prostate cancer patients
- RDaSH Children and Young People's Community Eating Disorder Service (CEDS)
- Boosting the Big Three in Diabetes Care: Foot, Eye & Kidney Checks
- Foundations of Health – Lunchtime Webinar Series 2025
- Non-Medical Prescribers bulletin update
- CYP Palliative and End of Life Transition Online Education Session for Primary Care
- ALABAMA Webinar
- Implementation of Jess’s Rule – three strikes and we rethink
News
NHS South Yorkshire Winter Covid & Flu Vaccinations Campaign Communications Toolkit 2025

Please find below a link to the NHS South Yorkshire Winter Covid & Flu Vaccinations Campaign Communications Toolkit 2025, which provides consistent messages and template assets to support public-facing communication to support the Winter Covid & Flu Vaccinations Campaign 2025.
Included within this toolkit is:
- Media release
- Social media posts and graphics
- Posters
- Digital screens for use on hospital, primary care and any other public facing screens
- Newsletter copy
- Website copy
- Video (more to follow)
- Winter Vaccines communications toolkit for people with a learning disability, autistic people, and people with severe mental illness
If you have any questions or need further support, please contact syicb.communications@nhs.net.
Thank you for your support in sharing these messages.
Supporting people with a Learning Disability, Autistic people, and people with Severe Mental Illness (SMI) to get their winter vaccines

Winter brings increased risks of flu, COVID-19, and associated complications. People with a learning disability, autistic people, and people with severe mental illness (SMI) are more vulnerable to poor health outcomes and have lower uptake of vaccinations compared to the general population.
To support equitable access across South Yorkshire, we have developed a South Yorkshire ICB Winter Vaccination Communications Toolkit for People with a Learning Disability, Autistic People, and People with Severe Mental Illness (SMI), which is part of the ICB Winter Vaccine toolkit in the item above.
We are asking all partners and stakeholders to:
- To watch the webinar from 2 September 2025 facilitated by NHSE Public Health Programmes Team (Screening & Immunisation Team)
- Promote winter vaccination messages using accessible materials and tailored communications. Flu vaccination: easy-read flu vaccination resources - GOV.UK Discover the health resource library
- Encourage eligible individuals to attend vaccination appointments, making sure reasonable adjustments are in place.
- Distribute resources locally (leaflets, Easy Read guides, videos, social stories, posters) through their networks and services.
- Support conversations about vaccine safety and benefits, addressing myths and hesitancy.
- Embed vaccination prompts (Making every contact count) into routine care and support planning (e.g., annual health checks, care reviews, community events).
- Feedback insights on barriers and enablers to uptake so that communications and delivery can be improved.
Thank you for your support in promoting vaccination uptake and reducing health inequalities this winter.
Learning Disability and Autism Programme
NHS South Yorkshire ICB
NHS England launches Medium Term Planning Framework

NHS England has published the Medium Term Planning Framework: Delivering Change Together 2026/27 to 2028/29, setting out a new approach to long-term planning and improvement across the NHS. The framework aims to move beyond short-term fixes, empowering local leaders to address fundamental challenges while improving care now. Co-produced with hundreds of NHS leaders, it focuses on restoring local ambition, accelerating access to primary and community care, and reducing waiting times. The framework builds on the 10-Year Health Plan and marks a major step toward a sustainable, community-focused NHS. Read the framework document here.
NHS South Yorkshire Interim CEO appointment
Chris Edwards has been appointed as Interim Chief Executive. Chris, who is currently Executive Place Director for Rotherham and has held the deputy CEO role since the inception of the ICB, has taken up the role after the retirement of Chief Executive Gavin Boyle earlier this month. The interim role will continue until 31 March 2026. Further updates, including a replacement for Chris as Executive Place Director for Rotherham, will be announced in due course.
Review of GP funding formula announced

\A review of GP funding formula, announced last week, is expected to deliver fairer distribution of funding and address health inequalities.
The six-month review will be conducted by the National Institute for Health and Care Research (NIHR). The review is expected to; identify a new allocation formula; assess the impact and feasibility of implementing it while ensuring it aligns to the government’s 10 Year Health Plan; and make an overall recommendation to replace the Carr-Hill formula.
Improving Outcomes for People with a Learning Disability

A new joint letter from the Secretary of State for Health and Social Care and Mencap highlights the vital role of primary care in improving health outcomes for people with a learning disability. It reinforces the importance of maintaining accurate learning disability registers and delivering high-quality annual health checks. Practices are asked to ensure eligible patients are included on the register and to share this message with all staff. Read the full letter here.
Expansion of the NHS Pharmacy Contraception Service – updated service specification and patient group directions

In anticipation of the expansion of the NHS Pharmacy Contraception Service to include emergency contraception, the updated service specification and patient group directions (PGDs) were published on NHS England’s website earlier this week. This will allow community pharmacy teams to prepare for the service expansion, including the delivery of PGDs by pharmacy technicians.
IT suppliers plan to update their systems ahead of go-live to allow contractors to record consultations appropriately and in line with the changes. The current service documents will be available on the NHSBSA website and will remain in place until the service commencement date for these enhancements is announced and authorised by NHS England.
Community pharmacy teams providing the NHS Pharmacy Contraception Service should read the updated service documents and sign the PGD authorisation sheet(s) in preparation for go-live.
Webinar for employers of Physician/Anaesthesia Associates
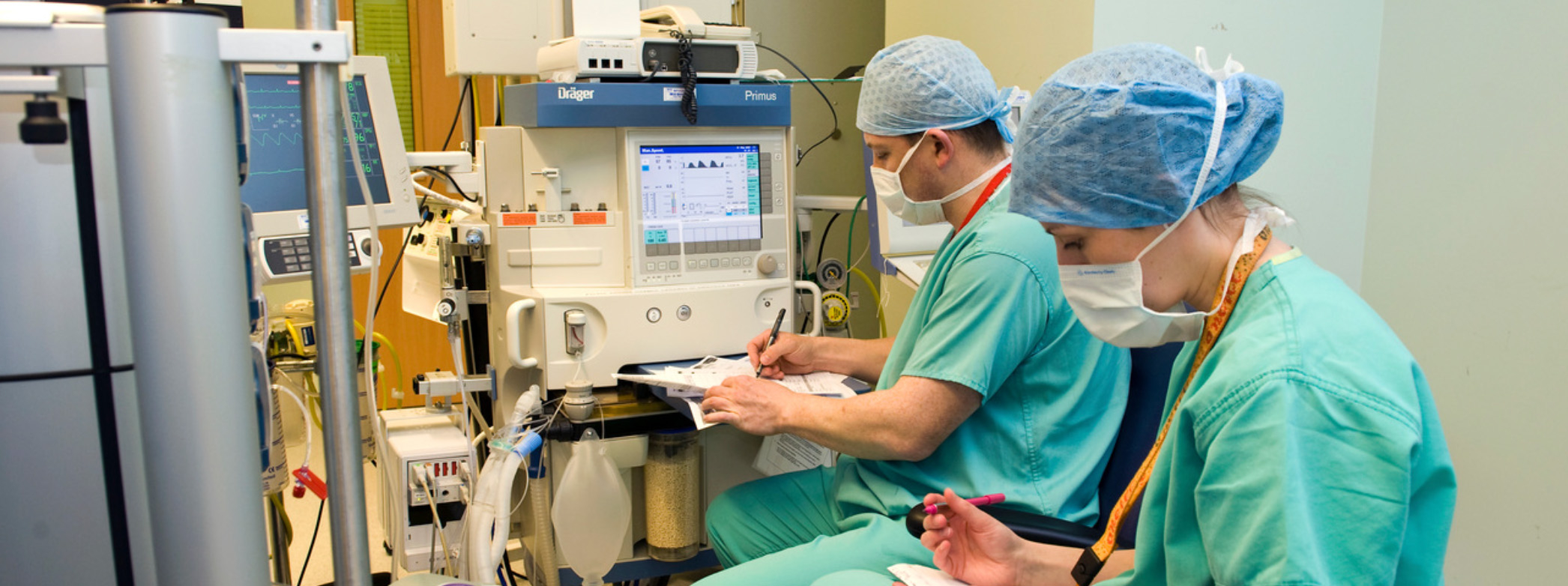
On Wednesday, 10 December 2025 at 12:30pm, we’ll be running a webinar for employers of PAs and AAs.
Sign up to join the webinar and send us your questions in advance. We’ll aim to answer as many as we can during the session.
The webinar will last approximately 90 minutes and will cover:
- Our approach to PA and AA regulation
- Recommendations from Gillian Leng’s independent review of the PA and AA professions in England
- Our guidance on supervision
- Good practice in clinical governance arrangements.
If you’re unable to attend but would like to hear about future webinars for PA and AA employers, you can register your interest below.
|
Sign up to join the webinar |
Register your interest for future webinars |
|
Sign up to join the webinar and send us your questions in advance |
Bassetlaw Hospice: Transfer of services

From 1 November 2025 the delivery of all palliative care services at Bassetlaw Hospice will transfer from Nottinghamshire Healthcare NHS Foundation Trust to the Bassetlaw Hospice Charity. This includes inpatient services, day services and clinical nurse specialist services. Since the Trust gave notice on the contract to deliver services at the Hospice in Autumn 2024, work has been taking place to ensure the safe and smooth transition, which includes staff working in these services transferring over to the Charity.
As part of the transition, from 13 October 2025, inpatient admissions to Bassetlaw Hospice will be suspended to allow for staff training and new systems to be set up. Day and outpatient services and clinical nurse specialist support will continue. People with palliative care needs will be offered support in their home with specialist and community support, in a care home or at John Eastwood Hospice, Mansfield or Beaumond House Hospice in Newark & Sherwood – depending on their wishes.
Referrals for an inpatient admission to John Eastwood Hospice can be made via 01623 622626 or for Beaumond House Hospice via 01636 610556 – please ask to be put through to the inpatient unit. Referrals out of hours for both hospices can be made via Call 4 Care on 01623 781899, option 2. This is a temporary measure until the inpatient unit at Bassetlaw Hospice opens again in November.
The referral pathway for Bassetlaw Hospice will change when the inpatient unit reopens, and we will advise you of the new process in the coming weeks.
We are pleased that Bassetlaw Hospice is taking on these services to enable support to continue for local residents.
For any queries, please contact Bassetlaw Hospice on 01777 200060 / bonney@bassetlawhospice.org
Digital pathways for follow-up with prostate cancer patients

Health Innovation Yorkshire and Humber is pleased to invite you to a short webinar presenting the findings of an NIHR-funded project assessing the use of Ascelus, a digital health app to remotely monitor patients recovering from prostate cancer treatment.
The project, which will be discussed, is an NIHR-funded collaborative project with the University of Sheffield and Sheffield Teaching Hospital focused on transforming the management of advanced prostate cancer in digital health. The project had a specific aim of increasing the representation of ethnic minorities.
We would greatly value your input in two ways:
1. Complete a short survey
We are inviting nurses, pharmacists, medical staff (including consultants and all grades in urology), uro-oncologists, and service managers to complete a short questionnaire (5–7 minutes). Your insights are vital to understanding current pathways, identifying challenges, and shaping future improvements in patient monitoring.
https://forms.office.com/e/8KYQPAjkg9
2. Join a webinar workshop
We are also hosting two interactive online workshops to share findings from the evaluation of the app, explore the role of digital health in prostate cancer care, and discuss opportunities for collaboration and future research.
Both sessions will cover the same content – please register for the time that best suits you:
Session 1: Monday 20 October, 12:30 – 14:00
Session 2: Friday 24 October, 14:00 – 15:30
Online (link to be provided after registration)
Register here: https://www.eventbrite.co.uk/e/webinar-on-remote-digital-monitoring-in-prostate-cancer-care-tickets-1673310178789?aff=oddtdtcreator
RDaSH Children and Young People's Community Eating Disorder Service (CEDS)

The Rotherham, Doncaster and South Humber, Children Young People’s Community Eating Disorder Service (CEDS) is a specialist, multidisciplinary service designed to deliver timely, evidence-based care to children and young people with eating disorders across our three localities, Doncaster, Rotherham and North Lincolnshire. Operating in line with NHS Long Term Plan priorities and NICE guidance, the service aims to reduce the need for inpatient admission and promote recovery within the least restrictive environment possible. We provide rapid triage, comprehensive assessment, and tailored interventions including medical monitoring, psychological therapies, dietetic support, and family-based treatment.
The team comprises psychology, specialist nursing, paediatrics, dietetics, family therapy and support workers, who work closely with families, schools, primary care, social care, and voluntary sector partners to create seamless, whole-system care pathways. By emphasising early intervention, proactive risk management and co-produced care plans, CEDS promotes recovery, enhances patient and family experience and optimises use of NHS resources.
Referral Pathway and Access
CEDS accepts both professional and self-referrals to maximise accessibility and support early intervention. There is no minimum weight or BMI threshold for acceptance, and no long referral form to help facilitate a seamless referral process. Referrals can be made by email or phone and are reviewed for risk promptly upon receipt.
Triage and Risk Stratification
In line with best practice and the Medical Emergencies in Eating Disorders (MEED) guidance, every referral is risk-assessed within 24 hours of receipt. The service aims to complete a full triage within this timeframe, engaging directly with the young person, their family and the referrer as appropriate. Following triage, accepted referrals are categorised as Emergency, Urgent, or Routine to ensure timely and proportionate care.
Consultation Offer for Professionals
To further enhance clinical decision-making and reduce inappropriate referrals, CEDS now provides weekly consultation sessions for professionals each Thursday morning. These sessions offer early advice and guidance where an eating disorder is suspected, enabling professionals to discuss cases prior to formal referral and ensuring that children and young people are directed to the most appropriate intervention without delay.
Contact
Email: rdash.ceds@nhs.net
Telephone: 03000 212 349
More information
See the attached GP information pack to find out more.
Boosting the Big Three in Diabetes Care: Foot, Eye & Kidney Checks

We are pleased to invite you to a practical, one-hour training session open to all primary care staff involved/interested in diabetes care.
- Thursday 27 November, 12:30-13:30. Register today by clicking here.
Hear directly from expert speakers as they share insight, tips, and real-world examples to help improve uptake of three vital care processes:
- Foot Checks – making every contact count
- Retinal Screening – closing the gap for non-attenders
- Urinary ACR Testing – quick, easy, and opportunistic approaches
Speakers:
- Dr Rajiv Gandhi, MD FRCP – Consultant Physician & NHSE Clinical Lead for Diabetes (Treatment & Care), NEY
- Kayleigh Christopher – Engagement Lead & Senior Screener Grader, Sheffield Diabetic Eye Screening Service
- Dan Clarke – CVD Prevention Lead (Joint), South Yorkshire ICB
This session will provide practical knowledge you can apply in your own role to help prevent serious complications such as amputations, sight loss, and kidney failure.
Any questions, please email Amy.moore39@nhs.net
Foundations of Health – Lunchtime Webinar Series 2025

Are you a GP, nurse or HCP who feels long-term condition management has become a cycle of medicines that don’t always help patients feel better? Want tools that go beyond prescribing?
Join this engaging webinar series designed for primary care professionals. Learn how simple, evidence-based approaches to sleep, stress, movement, and more can help prevent, and even reverse, chronic disease. Starts Tuesday 11 Nov, 12:30–13:15 and occurs weekly for 6 weeks on a Tuesday.
Enhance your clinical impact and personal well-being with strategies you can apply every day.
Recordings available via Diabetes SharePoint
For more information and other dates, see the attached flyer.
Non-Medical Prescribers bulletin update

There is a new process available for the registration of Non-Medical Prescribers (NMP) in Primary Care in South Yorkshire. The Process can be found on the Central Medicines Management Website by clicking here or by searching for ‘Non-Medical Prescribers’ in the South Yorkshire section of the website.
The new process has been developed to ensure the NHS Business Services Authority (NHSBSA) registration, deletion or amendment of all NMP requests are completed effectively for NMPs working within Primary Care, South Yorkshire, in line with the Non-Medical Prescribing Framework for Primary Care South Yorkshire.
The NMP Framework has also been reviewed and updated. This now includes a matrix for employers to understand their responsibilities towards maintaining prescribing governance (appendix 3) and an audit tool (appendix 2). These were developed by Anna Young and Kel Tyers to support all primary care non-medical prescribers. This was a joint piece of work between the Medicines Optimisation Team and the Primary Care Workforce and Training Hub.
If you need any further information or have any queries around the NMP Registration Process please email syicb.medsoptid@nhs.net
If you need any further information or have any queries or feedback around the NMP framework, matrix and audit tool please email Anna Young a.young@nhs.net
CYP Palliative and End of Life Transition Online Education Session for Primary Care

Bluebell Wood Hospice is hosting a CYP Palliative and End of Life Transition Education Session for Primary Care - Hosted by Bluebell Wood Hospice.
Join us virtually via the invite in your calendar at 13:00 on Tuesday, 30th September or follow the link below.
Meeting ID: 317 652 264 350 8
Passcode: KK2yy7nY
The aims of the session are:
- To provide an overview of the National and local picture relating to transitional care from children’s to adult services.
- To understand what the barriers are in the process of transition of young people with chronic health conditions into adult health services.
- To understand the role of Primary Care in supporting patients going through transition.
- To understand the role of the GP relating to Advanced Care Planning and explore best practice models.
By the end of the session, you will be able to:
- Have a clearer understanding of the local and national data relating to transition.
- Understand the challenges faced by YP and their families with chronic conditions when moving from paediatric to adult services.
- Reflect on the key challenges faced by Primary Care around transition.
- Be able to navigate the ACP process and RESPECT documentation.
Please feel free to forward this information to your colleagues.
ALABAMA webinar
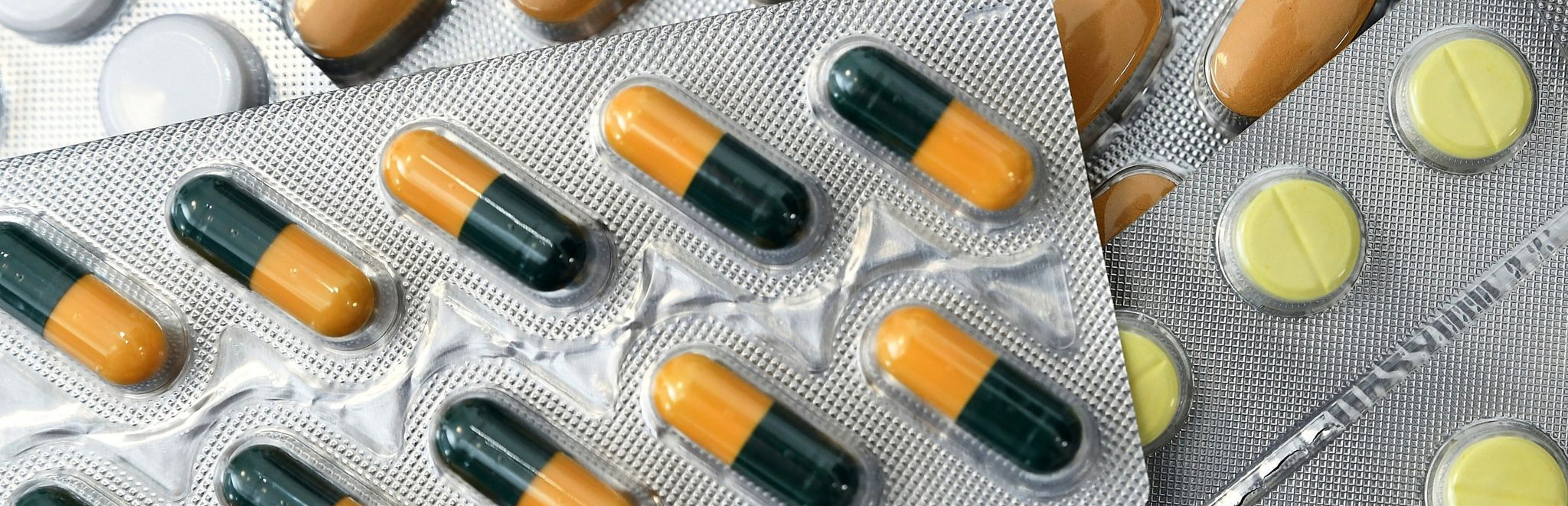
This November, the NIHR Yorkshire and Humber Regional Research Delivery Network (RRDN) hosts a Study Spotlight Webinar on the University of Leeds-led ALABAMA study – a primary care study into penicillin allergies.
The webinar takes place Monday, 3 November, 12-1 pm, online and provides an opportunity for attendees to learn more about ALABAMA’s findings and impact, which looked at whether individuals in primary care had a true penicillin allergy. The study’s results were recently published in The Lancet.
The webinar will be led by Prof Sue Pavitt and Dr Jon Sandoe, both of the University. Register your place.
Updates
Implementation of Jess’s Rule – three strikes and we rethink
NHS England and the Department of Health and Social Care have introduced Jess’s Rule, encouraging clinicians to review and re-evaluate cases where a patient presents for a third time with the same unresolved symptom or concern. The initiative aims to reduce diagnostic delays and improve patient safety through reflection, review, and rethinking. Read the letter here.
